Rural Hospitals are in deep trouble and Payer Mix is at least partially to blame
Understanding payer mix, one of the the most important concepts in healthcare economics, with an interactive Jupyter Notebook and a simple coffee shop example
Since 2005, a rural hospital closes in America every 30 days on average according to UNC’s SHEPS center program on Rural Hospital Closures. This trend is only accelerating. In 2020 according to Becker’s the rate of closure was every 18 days. This means more and more Americans, a fifth of whom live in rural America, have to go farther to receive inpatient hospital-level care. In addition, in many communities’ hospitals are not only a source of health but also a major employer. The question of why these hospitals close is a complex issue but the payer mix is a major factor.
I was inspired to combine my background in Hospital Revenue Cycle and Data Science to try and build a model to predict rural hospital closure. I spent the last semester of my MBA at Emory building a payer-mix estimation tool for rural hospitals based on demographic data. I then built a logistic regression to try and predict whether a hospital would remain open based on its payer mix. I found that the most powerful predictive variable for a rural hospital closing was the percentage of uninsured adults in the hospital’s coverage area or % Self-Pay. You can see the full paper and Tableau in the links down below
Check out the Tableau of the Rural Hospital Closure Paper
Interested in reading the full paper? Click Here
What is Payer Mix?:
Payer mix refers to a health systems distribution of third-party payer types. Typically, private insurance pays the most per episode, followed by Medicare, Medicaid, and lastly Self-Pay. Self-Pay is the industry term for patients without any insurance. Unlike any other business in America, hospitals must provide services to those who cannot pay. This is for good reason. Under EMTALA rules patients must be seen in the ER and treated for their acute conditions. The American College of Emergency Physicians describes this as an “unfunded mandate” .
Imagine instead of a hospital one was talking about a coffee shop that had to serve coffee to whoever came in. Each customer pays a different price depending on the plan they are a member of. The Private plan members pay $2 a cup. The Medicare members pay $1.2 a cup and the Medicaid members pay 90 cents a cup. Finally, there are folks who are not members of any plan aka Self-Pay members. They can pay 50 cents today but still needed to get coffee today. If coffee costs a business $1 per cup one can quickly see how the “mix” of these different types will cause the coffee shop to remain open or will cause it close.
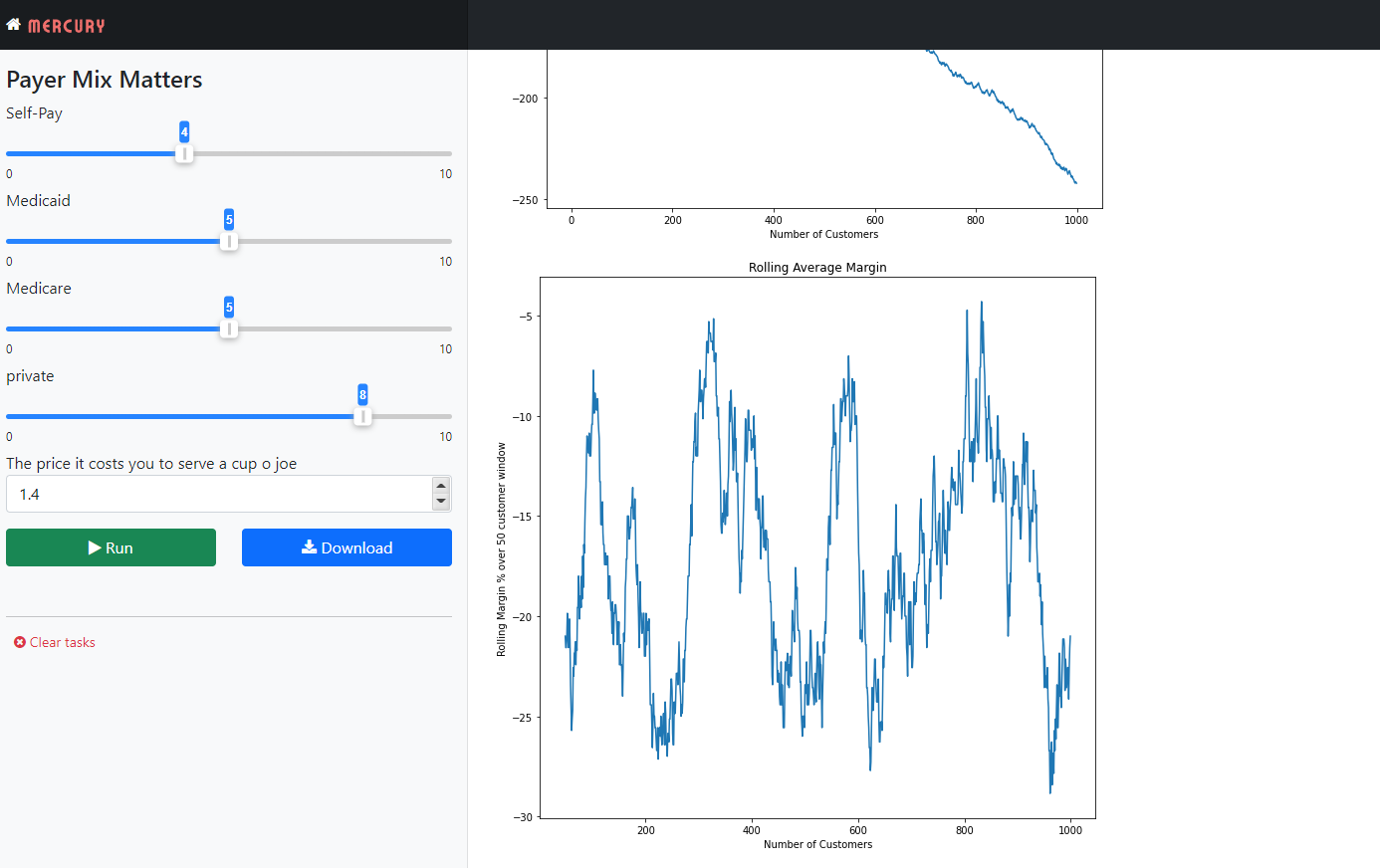
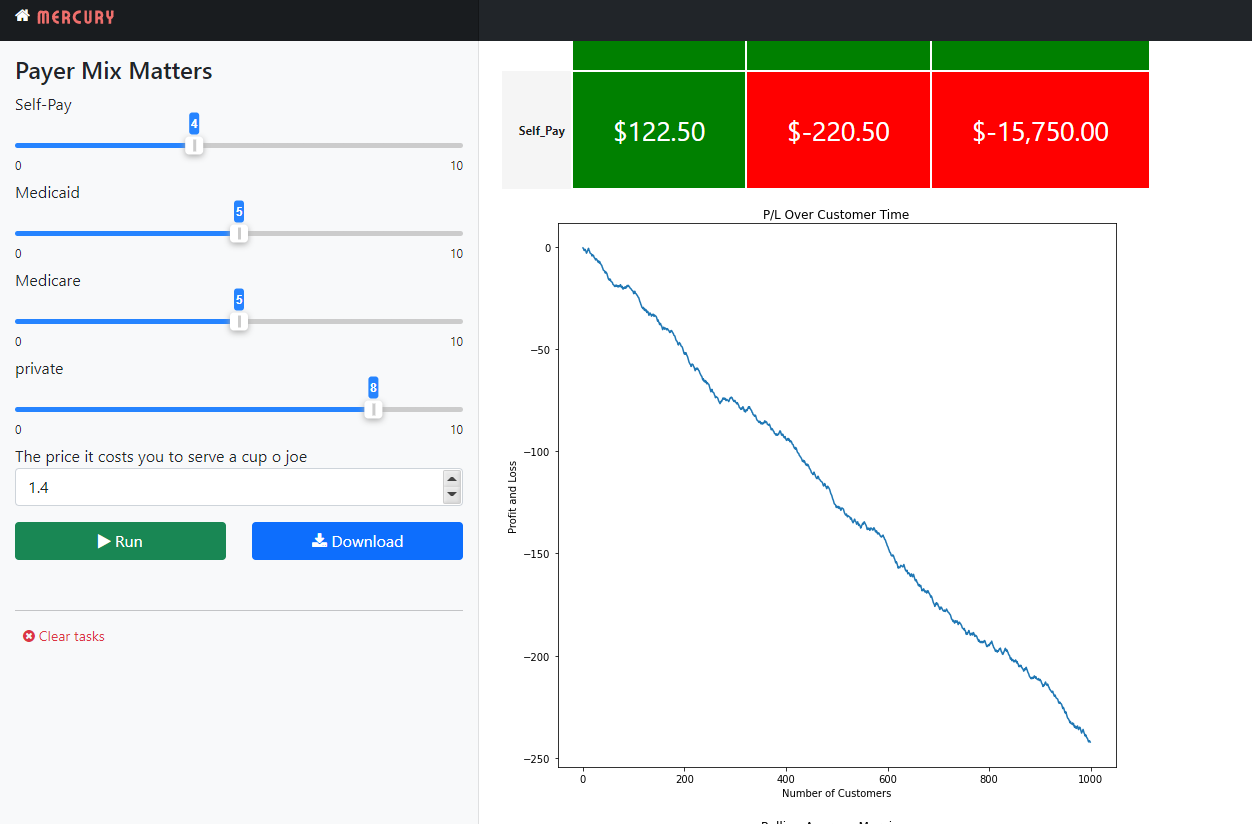
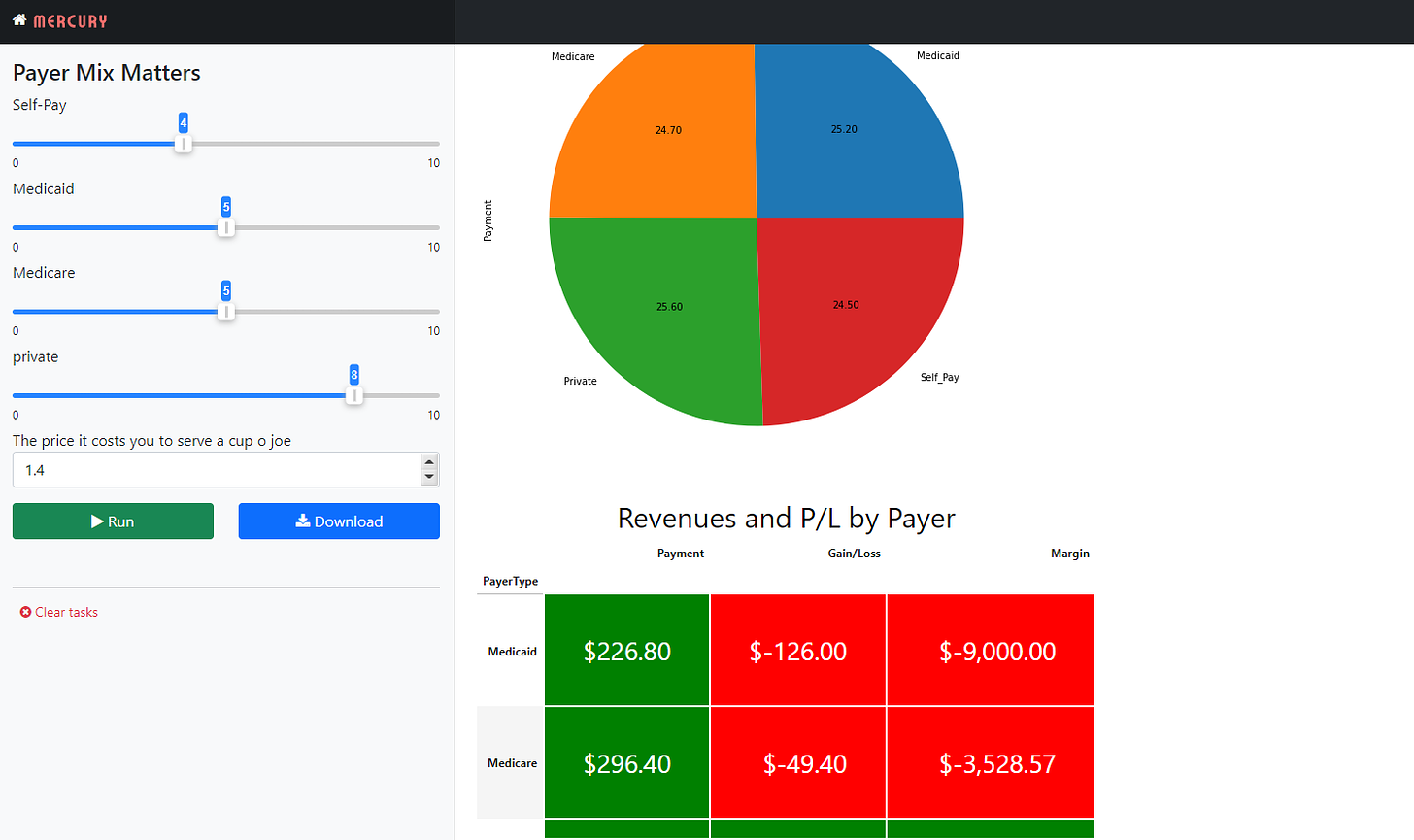
I’ve built an interactive Jupyter notebook with the Mercury library that allows you to test different payer mixes for this theoretical coffee shop and see the resulting Overall P/L,P\L By Quarter, and P/L by the payer.